In this blog I will outline the diagnostic process for tendinopathy. For detailed info and specifics on diagnosis for each lower limb tendon and lots of clinical assessment and management info check out upcoming courses in Melbourne, Sydney, Brisbane and the UK.
One of the issues with tendinopathy is that there is limited evidence and lots of areas with no consensus! This was clear at the recent ISTS 2014 biennial tendinopathy conference (which is a great event for those interested in tendons). At the end there was a recorded debate and consensus was near impossible to achieve for even basic questions like what is tendinopathy?
One of the key debated questions is how do we diagnose tendinopathy and what role does imaging have? Ask 5 clinicians and you will no doubt get 5 different answers. To some extent this is ok, maybe this tells us diagnosis will be a fluid process and depend on the tendon, the individual patient, and many other factors.
Here I will argue, mainly from clinical experience but also with some supporting evidence, that diagnosis is based on specific criteria. The absolute key is that diagnosis is based on multiple subjective and objective findings, not just a simple test or imaging finding. If you follow these criteria you virtually cannot go wrong.
So here are the 4 key steps…
1) Subjective question about pain
This is by far the most important criterion and for many tendon patients is enough to confirm a tendinopathy presentation. That is, you don’t even have to put your hands on the patient or look at imaging to be sure that you are dealing with a tendinopathy. There are 3 key clinical questions
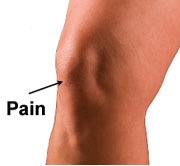
a) Where is the pain? We know that tendon pain is always super localized. For example, is patellar tendon pain should be exactly at the inferior patella pole (can be medial or lateral side), i.e. on the bone! (see Figure 1) If it is even 2cm further down the tendon from here we know that it is most likely coming from another tissue eg fat pad, PFJ, etc
Figure 1: Site of pain of patellar tendinopathy
b) Is there a clear stimulus (load) – response (pain) relationship? And does the stimulus involve energy storage and/or compressive load? Tendinopathy should be load related and we know that energy storage (ie walking, running, jumping) and compressive loads are implicated. These questions become difficult when patients have had years of tendon pain, but you can still determine whether pain fluctuation during this time are load related.
c) Is the pain behavior consistent with a tendinopathy? Tendon pain behaves in a predictable way. Pain ‘warms up’ or improves with activity, only to flare and be worse for hours or sometimes days after activity. Some tendons feel ‘stiff’ in the morning, consistently the Achilles and plantar fascia, less consistently some of the others.
2) Pain with load tests
With some patients we are lucky and the criteria above fit perfectly. Often, however, there may be an unclear history from the patient, the patient is unsure, or all the typical signs are not there – this leaves me unsure and the search for diagnostic evidence continues.
The next step is load tests aimed at provoking tendon pain. For each tendon there is a progression from low to higher and then very higher tendon load – this includes end range compressive as well as energy storage load. For example, the progression I use for suspected proximal hamstring tendinopathy includes double leg progressing to single and then long lever bridge, finally adding speed (Figure 2). If no symptoms were provoked a double leg progressing to single leg deadlift into end range can be provocative, especially when adding speed. Repeat 3-5x and stop when pain reproduced – rate the pain on a 0-10 numerical rating scale and this becomes a key reassessment marker pre-post manual therapy and rehab, and other treatment. It is not uncommon for a complete progression from low to very high load not to reproduce any symptoms, particularly in patients with stable or low level of symptoms – this does not necessarily mean that the tendon is not implicated, but it does mean you need to rely on other diagnostic criteria.
3) Exclude differential diagnoses
This step is particularly important when the subjective questions are unclear. E.g. perhaps the pain is slightly more diffuse then pin-point typical tendinopathy pain, or maybe the pain behavior does not add up to what you would expect for a tendon. In this instance it is critical to have an excellent knowledge of anatomy, potential associated versus differential diagnoses, and their signs and symptoms. After all, getting the right diagnosis and being able to identify associated diagnoses and their contribution really will set up all the management, and can save the patient unnecessary and ultimately ineffective treatment (unfortunately this does happen too commonly)
The key to excluding diagnosis is as discussed knowing how potential associated and differential diagnoses present (subjective information from questioning the patient) and special tests and palpation that can be used to include/exclude them. This process can be complex. Below I have included a table from a clinical narrative review paper I wrote last year with Craig Purdam on the assessment and management of proximal hamstring tendinopathy (Table 1). We also need to be mindful that central sensitization can present similarly to some differential diagnoses, eg sciatic nerve involvement in proximal hamstring tendinopathy.
Table 1: Associated/differential diagnosis of proximal hamstring tendinopathy
| Other diagnoses | Key features |
| Sciatic nerve at the ischial tuberosity | Sciatic tenderness at QFMay be provoked by hamstring slump, worse with hip adduction/IR
Diffuse thigh radiation of symptoms |
| Piriformis syndrome | Sciatic tenderness at piriformisMay be provoked with piriformis stretch/contraction or slump with adduction/IR
Diffuse thigh symptoms |
| Ischiogluteal bursitis | Pain on stretch or localised palpation Irritable symptoms with sitting?MRI or US confirmation |
| Lumbar facet arthorpathy, disc degeneration, radiculopathy | Diffuse leg referral?Inconclusive hamstring loading tests |
| Ischiofemoral impingement | Palpation tenderness over QF – variablePossible reproduction with femoral external rotation in hip neutral
MRI diagnosis if not responding |
| Unfused ischial growth plate (rare) | Avulsion history in teenage years MRI diagnosis if not responding |
| Apophysitis or avulsion | In younger athletesSudden incident, e.g. kicking |
| Chronic compartment syndrome of the posterior thigh (rare) | Pain that does not warm upDiffuse whole of hamstring discomfort |
| Posterior pubic or ischial ramus stress fracture | Female athletes, overtrainingTenderness over posterior pubic or ischial ramus |
4) Imaging to CONFIRM a diagnosis
We all know that imaging alone tells us very little about pain (see refs below). Therefore, imaging should not strictly be used to diagnose tendon pain, but can be a very useful adjunct in confirming which tissue may be involved in pain generation. Imaging is particularly useful when we have a clear idea from the subjective questions, load tests, and consideration of associated/differential diagnoses that there is something else going on and we want imaging confirmation. For example, pain in the region of the Achilles midportion that is on the medial side of the tendon may be related to plantaris, fat pad or paratenon involvement. Although there are specific signs and symptoms to differentiate these, imaging can be very useful to confirm, especially if it will influence the management, eg considering NSAID or injections, etc
I hope this clarifies or atleast gives a framework for the tendinopathy diagnostic process.
Please feel free to comment, would welcome discussion and thoughts
All the best
Peter
Key supporting references
Abate M, Gravare-Silbernagel K, Siljeholm C, et al. Pathogenesis of tendinopathies: inflammation or degeneration? Arthritis Research and Therapy. 2009;11:235.
Almekinders LC, Weinhold PS, Maffulli N. Compression etiology in tendinopathy. Clin Sports Med. 2003;22:703-710.
Cook J, Purdam C. Is compressive load a factor in the development of tendinopathy? British journal of sports medicine. 2012;46:163-168.
Kountouris A, Cook J. Rehabilitation of Achilles and patellar tendinopathies. Best Practice & Research in Clinical Rheumatology. 2007;21:295-316.
Malliaras P, Cook J. Patellar Tendons with normal imaging and pain: change in imaging and pain status over a volleyball season. Clinical Journal of Sports Medicine. 2006;16:388-391.
Malliaras P, Purdam C. Proximal hamstring tendinopathy assessment and management. Sport Health. 2014;32:21-29.